Elizabeth S. Pilcher, DMD
Department of Prosthodontics
College of Dental Medicine
Medical University of South Carolina
P.O. Box 250507
171 Ashley Avenue
Charleston, SC 29425
(803) 792-2341; Fax: (843) 792-1593
|
 |
Reprinted with the permission of the author, Elizabeth S. Pilcher, DMD
Paper presented at the 6th World Congress on Down Syndrome
October, 1997
Madrid, Spain
|
This study consists of a clinical and literature review of the special dental considerations unique to individuals with Down syndrome. The author is both a dentist and parent of a child with Down syndrome. Physical and orofacial characteristics of Down syndrome are discussed including the teeth, gingiva, tongue, palate, and occlusion. Incidences of dental decay and periodontal disease are discussed and how best to treat these diseases in persons with Down syndrome. Most if not all persons with Down syndrome have some type of occlusal disharmony. Techniques to help occlusal problems are discussed, including orthodontic therapy.
Medical problems associated with Down syndrome that can affect dental treatment are discussed. Also, social and emotional factors involved in dental treatment are covered, including techniques to help children with Down syndrome become cooperative dental patients. Information on how to choose the right dentist for your child and how to communicate effectively with the dental staff is given. Finally, information on proper home care and prevention of dental disease is covered, including information on the most recent dental products.
Introduction
Approximately one out of every 800-1,100 births results in an extra chromosome of the twenty-first group called
Trisomy 21, or Down syndrome. Affecting over 250,000 people in the U.S.
alone, this population has progressed tremendously over recent years to be able
to function in the mainstream of society. Inclusive school, work and community
settings are now becoming the norm for persons with Down syndrome. This
has resulted in a higher level of functioning for most of these individuals with
resulting increases in self-esteem and self-image. The demand for dental
care in persons with Down syndrome is increasing with this inclusive
trend. Most dental treatment for persons with Down syndrome can take place
in a general dental office with relatively minor adaptations. In
undergraduate dental training there is usually little or no exposure to treating
patients with disabilities, and general practitioners may be hesitant to treat
these patients with confidence. This paper will attempt to summarize the
unique characteristics associated with Down syndrome that influence the dental
care and treatment of this population.
Systemic factors influencing dental care
Although 40 to 50% of babies with Down syndrome are born with some type of
cardiac abnormality, most receive surgical correction within the first few years
of life. There is, however, an abnormally large percentage who develop
Mitral Valve Prolapse (MVP) by adulthood. The incidence of MVP in the
normal population is between 5 - 15%. Approximately 50%of adults with Down
syndrome have MVP requiring subacute bacterial endocarditis prophylaxis for
dental treatment (Barnett, Friedman, & Kastner, 1988). On third of
these adults with MVP do not have ascultatory findings, requiring diagnosis of
the MVP by echocardiogram. Patients with Down syndrome or their caregivers
may not be aware of the need for diagnostic echocardiography in adulthood.
A compromised immune system with a corresponding decrease in number of T
cells is characteristic of most individuals with Down syndrome. This
contributes to a higher rate of infections and is also a contributing factor in
the extremely high incidence of periodontal disease. Children with Down
syndrome often have chronic upper respiratory infections. These contribute
to mouth breathing with its associated effects of dry mouth (xerostomia) and
fissuring of the tongue and lips. There is also a greater incidence of
aphthous ulcers, oral candida infections and acute necrotizing ulcerative
gingivitis.
A reduced degree of muscle tone is generally found in Down syndrome.
This affects the musculature of the head and oral cavity as well as the large
skeletal muscles. The reduced muscle tone in the lips and cheeks
contribute to an imbalance of forces on the teeth with the force of the tongue
being a greater influence. This contributes to the open bite often seen in
Down syndrome. Additionally, reduced muscle tone causes less efficient
chewing and natural cleansing of the teeth. More food may remain on the
teeth after eating due to this inefficient chewing. Associated with the
low muscle tone is a ligamentous laxity seen throughout the body. This
causes hyperflexibility of the joints and is theorized that the ligaments around teeth may be influenced as well (Southern Assoc. of Institutional Dentists, p.4, 1994). A condition related to ligamentous laxity is that of Atlanto Axial Instability. The diagnosis and significance of this condition is controversial but is described as an increase in mobility between the C1 and C2 cervical vertebrae and may be seen in 10 - 20% of individuals with Down syndrome. If a patient has this instability, careful positioning in the
dental chair is required to avoid any potential harm to the spinal cord.
Persons with Down syndrome vary widely as to their degree of intellectual
impairment. Most have IQ's in the mild to moderate range and are able to
be treated in a normal setting. There is often a relatively severe delay
in language development. The patient with Down syndrome will probably
understand more than their apparent level of verbal skills. The assistance
of the patient's family or caregiver will be necessary in conveying to the
dentist and staff what level of communication should be used with the
patient. It may take a little extra appointment time to explain procedures
to the patient with Down syndrome, but once a level of trust is achieved they
are likely to be very cooperative patients.
Down syndrome is frequently seen in conjunction with other medical
problems. There is a higher incidence of epilepsy, diabetes, leukemia,
hypothyroidism and other conditions. Alzheimer's disease and Down syndrome
appear to have a strong connection to one another. The importance of a
thorough medical history including a work-up by a physician cannot be over
emphasized.
Orofacial features
The primary skeletal abnormality affecting the orofacial
structures in Down syndrome is an underdevelopment or hypoplasia of the
midfacial region. The bridge of the nose, bones of the midface and maxilla
are relatively smaller in size. In many instances this causes a prognathic
Class III occlusal relationship which contributes to an open bite (Vittek et al,
1994). Absence or reduction in size of the frontal and maxillary sinuses
is common.
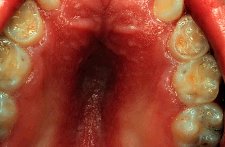 The incidence of mouth breathing is very high due to a
small nasal airway. The tongue may protrude and appear to be too
large. True macroglossia is rare, rather a relative macroglossia is found
where the tongue is of normal size but the oral cavity is decreased in size due to the underdevelopment of the mid-face. Upon examination the palate in a
person with Down syndrome appears to be narrow with a high vault. In
actuality the vault is of normal height but the sides of the hard palate are
abnormally thick. This creates less space in the oral cavity for the
tongue, affecting both speech and mastication. Speech pathologists can be
of help teaching correct tongue positioning and increasing the tone of the
orofacial musculature. In extreme cases, surgical reduction of the tongue
may be indicated (Margar-Bacal et al, 1987; Starmans & Bloem, 1991).
The incidence of mouth breathing is very high due to a
small nasal airway. The tongue may protrude and appear to be too
large. True macroglossia is rare, rather a relative macroglossia is found
where the tongue is of normal size but the oral cavity is decreased in size due to the underdevelopment of the mid-face. Upon examination the palate in a
person with Down syndrome appears to be narrow with a high vault. In
actuality the vault is of normal height but the sides of the hard palate are
abnormally thick. This creates less space in the oral cavity for the
tongue, affecting both speech and mastication. Speech pathologists can be
of help teaching correct tongue positioning and increasing the tone of the
orofacial musculature. In extreme cases, surgical reduction of the tongue
may be indicated (Margar-Bacal et al, 1987; Starmans & Bloem, 1991).
With age, both the tongue and the lips in people with Down syndrome tend to develop cracks and fissures. This is a result of chronic mouth breathing. Fissuring of the tongue can become severe and be a contributing factor in halitosis. Patients should be instructed to brush their tongue when they brush their teeth. Another result of chronic mouth breathing may be a decrease in saliva with a dry mouth. This reduces the natural cleansing that occurs in the oral cavity and may contribute to the development of caries.
Irritation at the corners of the mouth ("angular chelitis") may also be a result of mouth breathing.
The eruption of teeth in persons with Down syndrome is
usually delayed and may occur in an unusual order. (Mussig et al, 1990;
Fisher-Brandeis, 1989). The delay in eruption may be as long as two to three years. Although independence in feeding and the introduction
of food is encouraged in the toddler with Down syndrome, the diet may
need to be altered because there are not enough teeth to chew some
foods. There is an extremely high rate of missing teeth in
both the primary and permanent dentitions. Other irregularities such as microdontia and malformed teeth may be seen. However, in an oral cavity
with undersized bone structure, microdontia and missing teeth may be more of a
blessing than a problem. Severe crowding can occur in persons with Down
syndrome who have developed all of their permanent dentition (Ondarza et
al, 1995). In these cases, selective extractions under the supervision of an
orthodontist may be of benefit.
The roots of the teeth in patients with
Down syndrome tend to be small and conical. This is an
important factor when considering orthodontic tooth movement and also contributes to early
tooth loss in periodontal disease.
Dental disease
Historically the incidence of dental decay in persons
with Down syndrome has been reported to be extremely low. Recent studies,
however, have shown that while the incidence is lower, it is not as rare as once
thought and it certainly shouldn't be taken for granted that "these
patients won't get decay" (Barnett, 1986). Older studies of caries in
persons with Down syndrome used institutionalized populations whose diets were
controlled. These groups may not have had the exposure to cariogenic foods
at the rate of today's children with Down syndrome who are growing up at
home. The incidence is lower, however, and it is theorized that this may
be due to delayed eruption of the teeth, increased spacing between teeth or
possible differences in the chemical content of the saliva (Morinushi et al,
1995).
Today, children with Down syndrome should be educated in
proper oral hygiene, and receive the benefits of topical and systemic
fluoride. Occlusal sealants are also recommended. Decay in the
primary dentition should be properly treated. With the delay of the
permanent teeth and the high number of missing teeth, it is critical to maintain
the primary dentition as long as possible.
On the opposite end of the spectrum from caries is the
high rate of periodontal disease seen in Down syndrome (Shapira et al,
1991). Early, severe periodontal disease is often seen with onset in the
mid to late teen years. Some studies report an incidence of periodontal
disease to be between 90 and 96% of adults with Down syndrome. This is
thought to be related to a lowered host immune response due to the compromised
immune system in Down syndrome (Sohoel et al, 1995; Sohoel et al, 1992;
Reuland-Bosma, 1990; Shaw & Saxby, 1986). The amount of plaque and
calculus seen on the teeth is not proportionate ot the severity of the disease
(Yavuzyilmaz et al, 1993). The teeth most affected are the mandibular
incisors and maxillary molars. Good oral hygienee and semi-annual
prophylaxis appointments may not be enough to prevent the progression of
periodontal disease in these patients. Early, aggressive treatment is
needed. These patients may need to be seen as often as every three months
for scaling and root planing and may also benefit from the use of chlorhexedine
mouth rinse and possibly systemic antibiotic therapy (Stabholtz et al, 1991).
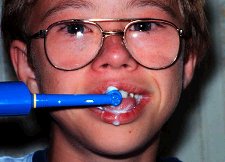 Obviously, good home care is essential in the management
of periodontal disease of this type. This may be difficult to achieve with
the intellectual impairment and decreased manual dexterity seen in Down
syndrome. Flossing may be very hard for these patients and instruction in
the use of a floss holder may be helpful. New mechanical tooth brushing
and flossing aids on the market may also be of help. It is important to be
sure that the patient's family or caregiver is educated in proper home care as well. Parents need to realize the importance of proper daily home care
because the child with Down syndrome may be resistant to tooth brushing.
Additionally, the age at which a child with Down syndrome can be expected to
take care of his/her own teeth may be much later than that of normal
children.
Obviously, good home care is essential in the management
of periodontal disease of this type. This may be difficult to achieve with
the intellectual impairment and decreased manual dexterity seen in Down
syndrome. Flossing may be very hard for these patients and instruction in
the use of a floss holder may be helpful. New mechanical tooth brushing
and flossing aids on the market may also be of help. It is important to be
sure that the patient's family or caregiver is educated in proper home care as well. Parents need to realize the importance of proper daily home care
because the child with Down syndrome may be resistant to tooth brushing.
Additionally, the age at which a child with Down syndrome can be expected to
take care of his/her own teeth may be much later than that of normal
children.
Treatment objectives
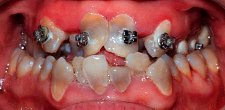 Treatment objectives for any population with developmental disabilities should be the same as that of normal patients.
Treatment plans may need to be adapted as necessary due to each individual's
condition, but the overall goal should be to provide as comprehensive treatment
as possible. Areas of dental care such as cosmetic dentistry,
orthodontics, prosthodontics, and reconstructive oral surgery should not be
ruled out simply because the patient has Down syndrome. With the numbers
of persons with Down syndrome working and living out in the community, there may
be many who desire and can handle some of the more extensive treatment options available
today.
Treatment objectives for any population with developmental disabilities should be the same as that of normal patients.
Treatment plans may need to be adapted as necessary due to each individual's
condition, but the overall goal should be to provide as comprehensive treatment
as possible. Areas of dental care such as cosmetic dentistry,
orthodontics, prosthodontics, and reconstructive oral surgery should not be
ruled out simply because the patient has Down syndrome. With the numbers
of persons with Down syndrome working and living out in the community, there may
be many who desire and can handle some of the more extensive treatment options available
today.
Behavior management
Good behavior in the dental office is learned. In a
population with delayed learning, this can be a challenge for the dentist and
staff. Dental treatment for children with Down syndrome may not be sought
out at an early age. There may be more pressing medical problems,
financial considerations or parents may want to wait until the child seems
mature enough to handle a visit to the dentist. Unfortunately this makes
it more difficult to teach proper home care and to develop a relationship with the child that will result in cooperative behavior during dental
treatment.
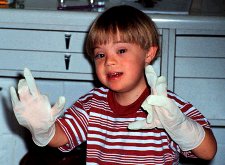 Determining the level of communication is very important
in developing a cooperative relationship with your patient with Down
syndrome. The level of receptive vs. expressive language may not be the
same. The patient's family or caregiver will be able to guide the dental
staff as to what level of communication is appropriate. It is important
that the dentist communicate directly with the patient whenever possible in
order to build a level of trust. It may be advantageous to have a parent
in the operatory during some early childhood visits. Finding out what
motivates the child with Down syndrome is also important. Something as
simple as receiving a pair of gloves and a mask at the end of the appointment may be all it takes to ensure cooperation. With more difficult patients requiring more extensive treatment, premedication and/or restraint may be necessary. However, most patients with Down syndrome can handle routine dental care with just a little more time and attention given during the appointment.
Determining the level of communication is very important
in developing a cooperative relationship with your patient with Down
syndrome. The level of receptive vs. expressive language may not be the
same. The patient's family or caregiver will be able to guide the dental
staff as to what level of communication is appropriate. It is important
that the dentist communicate directly with the patient whenever possible in
order to build a level of trust. It may be advantageous to have a parent
in the operatory during some early childhood visits. Finding out what
motivates the child with Down syndrome is also important. Something as
simple as receiving a pair of gloves and a mask at the end of the appointment may be all it takes to ensure cooperation. With more difficult patients requiring more extensive treatment, premedication and/or restraint may be necessary. However, most patients with Down syndrome can handle routine dental care with just a little more time and attention given during the appointment.
Scheduling appointments early in the day is beneficial as
both patient and operator are more rested. First appointments should be
for orientation only, and subsequent appointments may require a little more time than what is usually allowed. The patient's medical history should be
obtained prior to the first appointment. This allows for medical
consultation if necessary before any treatment begins.
Treating the older patient with Down syndrome may present
a different set of problems. There appears to be a higher incidence of
Alzheimer's disease in persons with Down syndrome. The average age of
onset of clinical symptoms is between 40 - 50 years (Sigal & Levine, 1993; Vicary & Caltigirone, 1990; Devenny et al, 1992). These patients will require a great deal of understanding and their level of cooperation may
decrease as the disease progresses.
Sleep Apnea
It is important that the dental health provider be aware
of the incidence of sleep apnea in the Down syndrome population. It has
been reported that the incidence of upper airway obstruction may be as high as 31% in children with Down syndrome (Stebbens et al, 1991). The decreased
airway size combined with lowered muscle tone predisposes these patients to
obstructive sleep apnea. Left untreated, obstructive sleep apnea can
further increase developmental delay and lead to pulmonary hypotension and
congestive heart failure. Symptoms of obstructive sleep apnea include
snoring, restless sleep and unusual sleeping positions. If a patient's
family or caregiver reports these symptoms, then referral to a sleep disorders clinic is indicated. Treatment ranges from occlusal repositioning
appliances, positive airway pressure and/or surgical correction.
Adenotonsillectomy in children with Down syndrome and sleep apnea has been
helpful in some cases (Bloch et al, 1990; Phillips & Rogers, 1988;
Silverman, 1988).
Summary
Dental care for the patient with Down syndrome can be
achieved in the general practitioner's office in most instances with minor
adaptations. Although this population has some unique dental care needs,
few patients require special facilities in order to receive dental
treatment. Adequate dental health care for persons with developmental disabilities is a major unmet health need. It is hoped that this review
will encourage general practitioners to be willing to provide comprehensive
dental care to their patients with Down syndrome.
References
Barnett M.L., Friedman D., & Kastner T. (1988). The prevalence of mitral valve prolapse in patients with Down syndrome: Implications for dental management. Oral Surgery Oral Medicine Oral Pathology, 66, 445-7.
Barnett M.L., Press, K.P., Friedman, D., & Sonnenburg, E.M. (1986). The prevalence of periodontitis and dental caries in a Down syndrome population. Journal of Periodontology, 57, 288-93.
Bloch K., Witztum, A., Wieser, H.G., Schmid, S., & Russi, E. (1990). Obstructive sleep apnea in a child with trisomy 21. Monatsschr ift Kinderheilkunde, 138, 817-22.
Devenny, D.A., Hill, A.L., Patxot, O., Silverman, W.P., & Wisniewski, K.E. (1992). Ageing in higher functioning adults with Down syndrome: an interim report in a longitudinal study. Journal of Intellectual Disabilities Research, 36, 241-50.
Fischer-Brandeis, H. (1989). The time of eruption of the milk teeth in Down's syndrome. Fortschritte derKeiferothopadie, 50, 144-51.
Margar-Bacal, F., Witzel, M.A., & Munro, I.R. (1987). Speech intelligibility after partial glossectomy in children with Down's syndrome. Plastic and Reconstructive Surgery, 79, 44-9.
Morinushi, T., Lopatin, D.E., & Tanaka, H. (1995). The relationship between dental caries in the primary dentition and anti S. Mutans serum antibodies in children with Down's syndrome. Journal of Clinical Pediatric Dentistry, 19, 279-83.
Müssig, D., Hickel, R., & Zschiesche, S. (1990). The eruption of decidious teeth in children with various forms of Down's syndrome and congenital heart defects. Deutche Zahnarzteblatt, 45, 157-9.
Ondarza, A., Jara, L., Bertonati, M.I., & Blanco, R. (1995). Tooth malalignments in Chilean children with Down's syndrome. Cleft Palate Craniofacial Journal, 32, 188-93.
Phillips, D.E., & Rogers, J.H. (1988). Down's syndrome with lingual tonsil hypertrophy producing sleep apnea. Journal of Laryngology & Otolaryngology, 102, 1054-5.
Reuland-Bosma, W. (1990). Periodontal disease in Down's syndrome. Ned Jijdscrift voor Tandheelkkunde, 97, 468-71.
Shapira, J., Stabholtz, A., Schurr, D., Sela, M.N., & Mann, J. (1991). Caries level, Streptococcus mutans counts, salivary pH and periodontal treatment needs of adult Down syndrome patients. Special Care Dentist, 11, 248-51.
Shaw, L., & Saxby, M.S. (1986). Periodontal destruction in Down's syndrome and in juvenile periodontitis; how close a similarity? Journal of Periodontology, 57, 709-13.
Sigal, M.J., & Levine, N. (1993). Down's syndrome and Alzheimer's disease. Journal of the Canadian Dental Association, 59, 823-29.
Silverman, M. (1988). Airway obstruction and sleep disruption in Down's syndrome. British Medical Journal, 296, 1618-9.
Sohoel, P.D., Johannessen, A.C., Kristofferson, T., Haugstvedt, Y., & Nilsen, R. (1992). In situ characteristics of mononuclear cells in marginal periodontitis of patients with Down's syndrome. Acta Odontologica Scandinavia, 50, 141-9.
Sohoel, P.D., Johannessen, A.C., Kristofferson, T., & Nilsen, R. (1995). Expression of HLA Class II antigens in marginal periodontitis of patients with Down's syndrome. European Journal of Oral Science, 103, 207-13.
Southern Association of Institutional Dentists (1994). Southern Assoc of Institutional Dentists Self-study Course: Module 3 Down syndrome.
Stabholtz, A., Shapira, J., Shur, D., Friedman, M., Guberman, R., & Selam M.N. (1991). Local application of sustained-release delivery system of chlorhexedine in Down's syndrome population. Clinical Preventive Dentistry, 13, 9-14.
Starmans J.L., & Bloem, J.J. (1991). Tongue reduction in children with Down's syndrome, a functional operation. Nederlands Tijdschrift Voor Geneeskunde, 135, 1963-6.
Stebbens, V.A., Dennis, J., Samuels, M.P., Croft, C.B., & Southhall, D.P. (1991). Sleep related upper airway obstruction in a cohort with Down's syndrome. Archives of the Disabled Child, 66, 1333-8.
Vicari. S., & Caltagirone, C. (1990). Alzheimer's disease and Down syndrome: a review. Rivista Neurologica, 60, 151-9.
Vittek. J., Winik, S., Winik, A., Sioris, C., Tarangelo, A.M., & Chou, M. (1994). Analysis of orthodontic anomalies in mentally retarded developmentally disabled persons. Special Care Dentist, 14, 198-202.
Yavuzyilmaz, E., Ersoy, F., Sanal, O., Tezcan, I., & Ercal, D. (1993). Neutrophil chemotaxis and periodontal status in Down syndrome patients. Journal of Nihon University School of Dentistry, 35, 91-5.
Revised: May 3, 1999.
 The incidence of mouth breathing is very high due to a
small nasal airway. The tongue may protrude and appear to be too
large. True macroglossia is rare, rather a relative macroglossia is found
where the tongue is of normal size but the oral cavity is decreased in size due to the underdevelopment of the mid-face. Upon examination the palate in a
person with Down syndrome appears to be narrow with a high vault. In
actuality the vault is of normal height but the sides of the hard palate are
abnormally thick. This creates less space in the oral cavity for the
tongue, affecting both speech and mastication. Speech pathologists can be
of help teaching correct tongue positioning and increasing the tone of the
orofacial musculature. In extreme cases, surgical reduction of the tongue
may be indicated (Margar-Bacal et al, 1987; Starmans & Bloem, 1991).
The incidence of mouth breathing is very high due to a
small nasal airway. The tongue may protrude and appear to be too
large. True macroglossia is rare, rather a relative macroglossia is found
where the tongue is of normal size but the oral cavity is decreased in size due to the underdevelopment of the mid-face. Upon examination the palate in a
person with Down syndrome appears to be narrow with a high vault. In
actuality the vault is of normal height but the sides of the hard palate are
abnormally thick. This creates less space in the oral cavity for the
tongue, affecting both speech and mastication. Speech pathologists can be
of help teaching correct tongue positioning and increasing the tone of the
orofacial musculature. In extreme cases, surgical reduction of the tongue
may be indicated (Margar-Bacal et al, 1987; Starmans & Bloem, 1991).
 Obviously, good home care is essential in the management
of periodontal disease of this type. This may be difficult to achieve with
the intellectual impairment and decreased manual dexterity seen in Down
syndrome. Flossing may be very hard for these patients and instruction in
the use of a floss holder may be helpful. New mechanical tooth brushing
and flossing aids on the market may also be of help. It is important to be
sure that the patient's family or caregiver is educated in proper home care as well. Parents need to realize the importance of proper daily home care
because the child with Down syndrome may be resistant to tooth brushing.
Additionally, the age at which a child with Down syndrome can be expected to
take care of his/her own teeth may be much later than that of normal
children.
Obviously, good home care is essential in the management
of periodontal disease of this type. This may be difficult to achieve with
the intellectual impairment and decreased manual dexterity seen in Down
syndrome. Flossing may be very hard for these patients and instruction in
the use of a floss holder may be helpful. New mechanical tooth brushing
and flossing aids on the market may also be of help. It is important to be
sure that the patient's family or caregiver is educated in proper home care as well. Parents need to realize the importance of proper daily home care
because the child with Down syndrome may be resistant to tooth brushing.
Additionally, the age at which a child with Down syndrome can be expected to
take care of his/her own teeth may be much later than that of normal
children.
 Treatment objectives for any population with developmental disabilities should be the same as that of normal patients.
Treatment plans may need to be adapted as necessary due to each individual's
condition, but the overall goal should be to provide as comprehensive treatment
as possible. Areas of dental care such as cosmetic dentistry,
orthodontics, prosthodontics, and reconstructive oral surgery should not be
ruled out simply because the patient has Down syndrome. With the numbers
of persons with Down syndrome working and living out in the community, there may
be many who desire and can handle some of the more extensive treatment options available
today.
Treatment objectives for any population with developmental disabilities should be the same as that of normal patients.
Treatment plans may need to be adapted as necessary due to each individual's
condition, but the overall goal should be to provide as comprehensive treatment
as possible. Areas of dental care such as cosmetic dentistry,
orthodontics, prosthodontics, and reconstructive oral surgery should not be
ruled out simply because the patient has Down syndrome. With the numbers
of persons with Down syndrome working and living out in the community, there may
be many who desire and can handle some of the more extensive treatment options available
today.
 Determining the level of communication is very important
in developing a cooperative relationship with your patient with Down
syndrome. The level of receptive vs. expressive language may not be the
same. The patient's family or caregiver will be able to guide the dental
staff as to what level of communication is appropriate. It is important
that the dentist communicate directly with the patient whenever possible in
order to build a level of trust. It may be advantageous to have a parent
in the operatory during some early childhood visits. Finding out what
motivates the child with Down syndrome is also important. Something as
simple as receiving a pair of gloves and a mask at the end of the appointment may be all it takes to ensure cooperation. With more difficult patients requiring more extensive treatment, premedication and/or restraint may be necessary. However, most patients with Down syndrome can handle routine dental care with just a little more time and attention given during the appointment.
Determining the level of communication is very important
in developing a cooperative relationship with your patient with Down
syndrome. The level of receptive vs. expressive language may not be the
same. The patient's family or caregiver will be able to guide the dental
staff as to what level of communication is appropriate. It is important
that the dentist communicate directly with the patient whenever possible in
order to build a level of trust. It may be advantageous to have a parent
in the operatory during some early childhood visits. Finding out what
motivates the child with Down syndrome is also important. Something as
simple as receiving a pair of gloves and a mask at the end of the appointment may be all it takes to ensure cooperation. With more difficult patients requiring more extensive treatment, premedication and/or restraint may be necessary. However, most patients with Down syndrome can handle routine dental care with just a little more time and attention given during the appointment.