Child & Family Psychiatric Unit
Ottawa General Hospital, Ottawa, Canada
G. Mintsioulis, M.D.
1995 National Association for Dual Diagnosis II Conference
NADD Founder and Executive Director
132 Fair Street
Kingston, NY 12401
(914) 331-4336
|
Chrissoula Stavrakaki, M.D., Ph.D., FRCPC Child & Family Psychiatric Unit Ottawa General Hospital, Ottawa, Canada G. Mintsioulis, M.D. 1995 National Association for Dual Diagnosis II Conference |
Reprinted with the permission of Robert J. Fletcher, DSW, ACSW NADD Founder and Executive Director 132 Fair Street Kingston, NY 12401 (914) 331-4336 |
| Down's | Non-Down's | |
|---|---|---|
| Number | 5 | 5 |
| Female/Male | 2/3 | 2/3 |
| Age/Years | Mean 30 Range 24-30 |
Mean 30 Range 22-40 |
Chart 1
Life Events
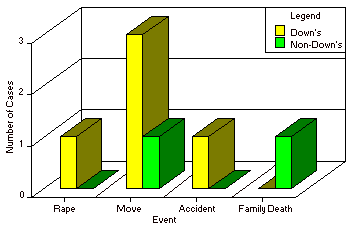
Chart 2
Symptom Presentation of Down's vs Other
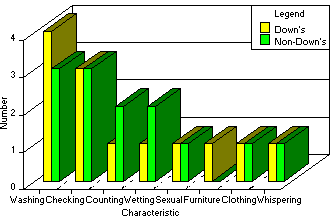
Chart 3
Degree of Mental Retardation
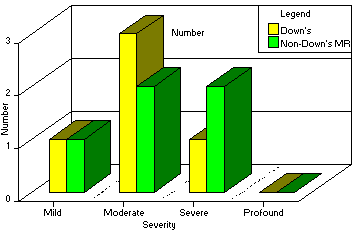
Chart 4
Drugs Used in Treatment of Non-Down's
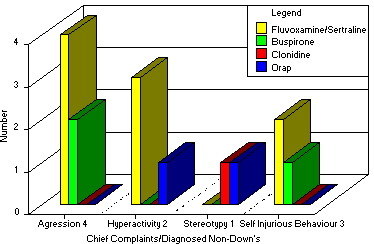
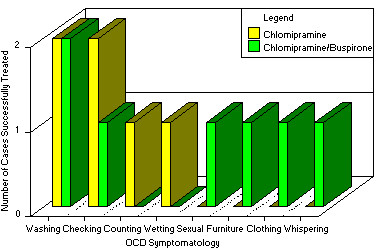
Chart 5
Treatment of Down's with OCD