Douglas Brockmeyer, MD
Division of Pediatric Neurosurgery
Primary Children's Medical Center
100 N. Medical Dr.
Salt Lake City, UT 84113, USA
Editor, Nepal Journal of Neuroscience
|
Nepal Journal of Neuroscience 2(1):52-58, 2005 Jan Douglas Brockmeyer, MD Division of Pediatric Neurosurgery Primary Children's Medical Center 100 N. Medical Dr. Salt Lake City, UT 84113, USA |
Reprinted with the permission of Mohan R. Sharma, MD Editor, Nepal Journal of Neuroscience |
Down's syndrome, is the most common inherited chromosomal disorder in humans occurring in 1.5 in every 1,000 live births and is characterized by multiple neurological as well as nonneurological abnormalities. The issue of craniovertebral instability in Down's syndrome patients is a very controversial topic. Multiple studies and editorials have been written over the last two decades and much of the information is conflicting and confusing. The goal of this review is to provide a rational synthesis of this previous work and provide recommendations by which parents of Down's syndrome patients, pediatricians, family practitioners and other health professionals may make intelligent choices regarding screening of Down's syndrome patients. It is a second goal of this review to synthesize the surgical data on this topic and provide recommendations for anesthesiologists, otolaryngologists, orthopedic surgeons and neurosurgeons.
Key Words: craniovertebral instability, Down's syndrome, pediatrics
Trisomy 21, or Down's syndrome, is the most common inherited chromosomal disorder in humans. It occurs in 1.5 in every 1,000 live births and is characterized by mild to moderate mental retardation, craniofacial-skull base abnormalities, cardiovascular disorders, gastrointestinal problems and immunological deficiency. In 1983, the Special Olympics mandated that routine radiographic cervical spine screening should be performed in all Down's syndrome patients before participating in "high-risk" sports. This decision was supported by the American Academy of Pediatrics in 1984.1 Since then, the issue of craniovertebral instability in Down's syndrome patients has developed into a very controversial topic. Multiple studies and editorials have been written over the last two decades and much of the information is conflicting and confusing. The goal of this review is to provide a rational synthesis of this previous work and provide recommendations by which parents of Down's syndrome patients, pediatricians, family practitioners and other health professionals may make intelligent choices regarding screening of Down's syndrome patients. It is a second goal of this review to synthesize the surgical data on this topic and provide recommendations for anesthesiologists, otolaryngologists, orthopedic surgeons and neurosurgeons. These decisions concern not only when screening studies are performed, but also when deciding which patients are at high risk and which patients should undergo surgery.
The traditional concepts regarding normal craniovertebral junction biomechanics have been most elegantly described by White and Panjabi.28 Stability at the occipital-atlantal (O A) level is provided by several elements which provide major degrees of support and two elements which provide minor degrees of support. The major supporting structures include the cup-shape joints at the atlanto-axial (AA) articulation. These include the occipital condyles and superior articular surface of the ring of C1. The capsular ligaments surround and anchor the joints of the OA space and are supplemented by the anterior and posterior atlanto-occipital membranes. The tectorial membrane, a continuation of the posterior longitudinal ligament, also provides significant structural support at this level. The alar and apical ligaments provide minor degrees of support for this joint.
At the AA joint, White and Panjabi describe two major structures supplying stability.28 These include the bony integrity of the odontoid process and the integrity of the transverse ligament. Both of these together provide the vast majority of stability that is necessary at this level. The alar ligaments, which attach from the dens to the ring of C1 and the foramen magnum, provide a minor degree of support at this level. They essentially act as check ligaments during periods of rotation.
Craniovertebral motion, as described by White and Panjabi,28 is traditionally broken down into directions of flexion/extension, one side lateral bending and one side lateral rotation. For the OA joint, 25° of motion is provided for flexion/extension, 5° of motion for one side lateral bending and 5° of motion for one side axial rotation. For the AA joint, 20° of flexion/extension occurs, 5° of one side lateral bending and 40° of one side axial rotation. It is clear from these data that the OA joint provides mostly flexion and extension while the AA joint provides mostly axial rotation with a smaller degree of flexion and extension. These concepts are important to remember when the issues of multidirectional instability are discussed later.
Next, one must consider what factors make the craniovertebral joint unstable in Down's syndrome patients. At the OA joint, two factors may account for this. One is abnormal joint anatomy, where the cup-shaped joints are replaced by flat or "rocker bottom" type joints. The second factor is ligamentous laxity in any or all of the important OA ligaments that provide structural stability at that level. At the AA joint, bony anomalies such as os odontoideum as well as laxity of the transverse ligament will result in instability at this level. Either one or both working together is sufficient to cause instability at this joint.
In 1983, after careful review of the medical literature, the Special Olympics mandated that all Down's syndrome patients would have cervical spine screening prior to participation in "high- risk" sporting activities. Cervical spine screening was defined as plain lateral radiographs in the neutral flexion and extension positions. High-risk sports included diving, swimming, pentathlon, high jump, etc. If the atlanto-dens interval (ADI) was greater than 4.5mm, then that child could not participate in high risk sporting activities at the Special Olympics. No mention is made in their report of why the arbitrary distance of 4.5mm was chosen as the cut-off. The Special Olympics advisory board also felt that no follow-up films were necessary if the atlanto-dens interval was less than 4.5mm unless symptoms consistent with myelopathy occur. If the ADI was greater than 4.5mm, then surgical stabilization should be considered, according to the board.
As a result of this mandate, thousands of children with Down's syndrome, who were either presently participating in the Special Olympics, or planned to participate, were affected. In 1984, the American Academy of Pediatrics Committee on Sports Medicine reviewed the Special Olympics mandate in the available literature.1 At that point, they endorsed the guidelines and also stated that more study of this controversial topic is needed. In 1995, the American Academy of Pediatrics again reviewed the situation regarding the Special Olympics mandate.2 They noted that since the Special Olympics will not lift the screening guidelines, then "identifying patients who have complaints consistent with symptomatic spinal cord injury is a greater priority than obtaining radiographs".28 It is also assumed from the article, but not directly stated, that once cervical fusion is successful, then full participation in "high-risk" activities may be performed. They also stated that better screening studies are needed to provide more detailed information about which patients are at risk for developing sudden catastrophic injury as a result of craniovertebral instability. To that end, the Academy reviewed 41 separate cases regarding sudden, significant spinal cord injuries in children with Down's syndrome.5,6,13,14,15,25,29 These cases provide ample documentation that those injuries can occur, but does not provide illumination as to how to prevent or treat them. In their summary they state: "Almost all symptomatic patients had their first radiograph at the time the symptoms were recognized, so it is generally unknown whether asymptomatic atlanto-axial instability (AAI) progresses to symptomatic AAI with or without trauma." Therefore, it remains unknown whether screening studies for Special Olympics participation is an effective way to prevent significant spinal cord injury in Down's syndrome patients.
Depending on the study, 10-30% of all Down's syndrome patients have evidence of AAI. The incidence of instability depends on: 1) the population studied (adult versus pediatric populations, or mixed, single institution studies versus multi-institution studies); 2) the imaging study used (plain radiographs, computed tomography (CT), or magnetic resonance imaging (MRI)); 3) the measurements used to determine instability, ADI, Neural canal width (NCW), Powers ratio, etc.); 4) whether magnification on the x-ray is corrected for; and 5) whether bony anomalies seen on the radiographs are also accounted for.
In 1987, Pueschel and Scola,19 described the radiographic findings of 404 patients with Down's syndrome. They described a 14.6% incidence of AAI in that population and a 13.1% incidence of asymptomatic instability. One and one half percent of the population, or six patients, showed symptomatic AAI and subsequently received operative stabilization. They felt that there was a "good correlation" with the ADI and NCW as measured by plain radiographs (p<0.005). The ADI is defined as the distance between the posterior surface of the anterior arch of C1 and the anterior surface of the dens. The NCW is defined as the distance between the posterior surface of the dens to the anterior surface of the posterior arch of C1. However, their correlation coefficients were rather poor with flexion r=-.353 and extension r=-.358.
One hundred and thirty seven Down's syndrome patients were described by Roy, et al., in 1990.22 They found a 10.2% incidence of instability using the ADI criteria. They also felt that radiological abnormalities found in this population did not correlate with neurologic abnormalities. Pueschel, et al.,21 again in 1990, described 78 Down's syndrome patients compared to 39 age match controls. They found that there was a higher incidence of cervical spine abnormalities in Down's syndrome patients seen on plain film though most of these anomalies were biomechanically insignificant. However, it was interesting to note there was a higher incidence of bony anomalies in the patients with AAI.
Selby, et al.,24 found in 135 patients with Down's syndrome that assessing AAI using the ADI did not correlate with myelopathic findings. The CT findings in 20 patients out of 59 with AAI were described by Pueschel, et al., in 1992.18 Their findings showed that the ADI measured less on CT scan than plain film. In addition, 9 of the 20 patients studied had bony anomalies. Two of these anomalies included os odontoideum, but the others were biomechanically insignificant.
In the only study using MRI to measure canal width, White, et al.,27 in 1993 described 17 patients with Down's syndrome. They measured the ADI and neural canal width (NCW) in plain films and correlated them with the subarachnoid space available for the spinal cord at the AA level. They found a high correlation between NCW and subarachnoid space diameter on MRI, but found that the ADI did not correlate well. Their recommendations are that the NCW and the ADI should be measured routinely in all cervical spine plain films studies. They also felt that a low NCW (less than 14mm) or evidence of occipital cervical instability should lead to an MRI before activity is restricted. Ferguson, et al.,8 in 1987 studied the plain radiographs in 84 patients with Down's syndrome. They measured the ADI and NCW. Seventeen of the 84 patients had subluxations and 5 of those were symptomatic. Sixty-seven of the patients were placed into a "non-subluxator" group and 18 of those patients were symptomatic. There was no statistical difference between the incidence of symptomatic myelopathy between the 'subluxator' and 'non-subluxator' group. In addition, seven MRI's were performed on the symptomatic 'non-subluxator' group. All of them were negative for spinal cord pathology. Four MRI's were performed on the symptomatic 'subluxator group' and only one of the four studies was positive for spinal cord pathology. Their conclusions were that AAI might not account for all central nervous system symptoms seen in Down's syndrome patients.
Thirty-two Down's syndrome patients with a 13-year follow-up were reported by Burke in 1985.4 The ADI was measured on plain cervical spine films in all patients. Their conclusions were that over time the average ADI increased to a significant degree (p<0.005). However, there was some crossover between groups over time. Specifically, some of the 'subluxators' became 'non-subluxators' and vice versa. The fact that crossover occurred and the small number of patients sampled holds this study suspect. Ninety-five Down's syndrome patients were followed anywhere between three to six years and described by Pueschel, et al., in 1987.17 They noted no changes in the ADI or clinical status over that time in this patient population. Ohsawa, et al.,16 described the five year follow-up in 69 patients "without separate odontoid processes" in 1989. This study is the only report to separate patients with os odontoideum from those with pure ligamentous laxity. The authors found that the ADI, measured in neutral, flexion and extension positions, "decreased with time when compared with the one at the initial examination ", but the difference was not statistically significant. In addition, there was no statistically significant difference in NCW measurements over time.
In another study, 141 patients were studied every three to four years with plain films on four separate occasions by Pueschel, et al.20 One hundred and thirty one out of 141 patients had minor ADI changes over time. Eleven out of the 141 patients had 2-4mm ADI changes, but no clinical symptoms were noted. As in previous studies, some crossover was seen between the 'subluxator' and 'nonsubluxator' groups with time. They recommended careful follow-up for this group of patients.
Morton, et al.,12 in 1995 described a five-year follow-up of 90 Down's syndrome patients. They found an overall decrease in the ADI over time and no new cases of AAI. The three year follow-up of Ferguson, et al.'s8 84 patients showed no change in ADI or neural canal width over time. They also found that there was no crossover between the 'subluxator' and 'non-subluxator' groups during their followup interval.
Taken together, the weight of evidence suggests that Down's syndrome patients with pure atlanto-axial ligamentous laxity and no bony anomalies undergo little or no change in the degree of their subluxation over time. These findings have important implications for the counseling of families and their Down's syndrome children. First, if plain radiographic screening has confirmed that significant instability is not present, then the child's activity need not be restricted and further screening is not indicated. However, the age of the patient when the screening is performed is still a controversial topic and further investigation is required. It seems reasonable that if no instability is discovered by the age of 10 years, then screening may be stopped. Second, if the screening process uncovers atlanto-axial or occipito-atlantal instability, then the finding should be addressed by a qualified individual, preferably a physician with experience in evaluating and treating disorders of the pediatric spine, including Down's syndrome.
The concept of OA instability in Down's syndrome is not new, but had been relatively overlooked until recently. In 1990, Treadwell, et al.,26 described 64 patients with Down's syndrome. 61% had greater than 4mm subluxation at the OA level. 21% had a greater than 5mm ADI between flexion and extension films. Three of the 15 unstable patients seen in their studies had os odontoideum. Treadwell makes the important point that rotatory instability may also be present in this population.26 Their study emphasized multidirectional instability as a potentially significant finding in this population. Menezes and Ryken10 in 1992 described a surgical experience in 18 symptomatic patients with Down's syndrome. 50% of his patients had occipital C1 instability and 50% of them had C1-2 rotatory subluxation. Three out of the 18 patients had os odontoideum. After dorsal fusion, two of the 18 patients had irreducible basilar invagination and required transoral resection of the odontoid for ventral pathology.
It is a fact that Down's syndrome patients frequently require upper airway procedures. This includes both adenoidectomies and tympanostomies. During these procedures, extreme neck positions are required, which consists of significant extension during the adenoidectomy and 90° rotation during the tympanostomy. A review in the otolaryngologic literature by Harley and Collins9 in 1994 strongly recommended that all patients undergo preoperative screening before otolaryngologic procedures. They felt that "the small screening cost is justifiable in this population".
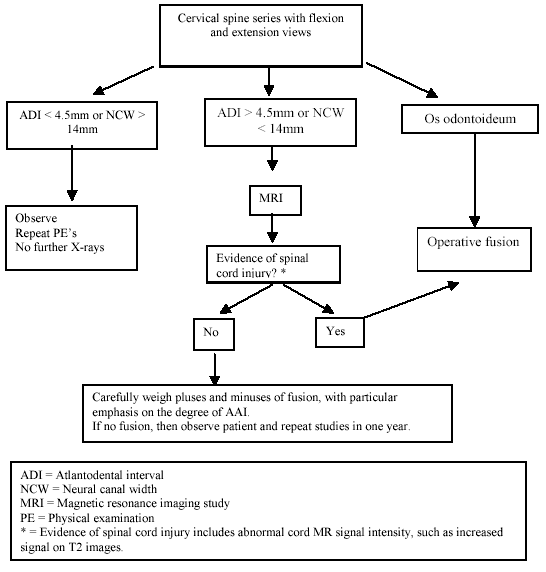 |
| Figure 1. Clinical management algorithm for asymptomatic atlanto-axial instability in Down's syndrome |
A survey of 171 pediatric anesthesiologists was reported in 1995.11 Of the pediatric anesthesiologists who responded, 18% obtained preoperative radiographs on asymptomatic Down's syndrome patients prior to surgery. 74% obtained preoperative radiographs and/or subspecialty consultation on patients who had myelopathic symptoms. It seems that the vast majority of pediatric anesthesiologists are aware of the need for preoperative radiographic studies or consultation prior to administering a general anesthetic. It has been our experience that general anesthesia relaxes muscle tone enough that previously unsuspected instabilities may be uncovered. We have encountered a case of AAI which was diagnosed preoperatively and then after general anesthetic was induced, an unsuspected OA instability was uncovered. This patient eventually went on to require an occipital cervical fusion. Awareness of these matters is paramount in avoiding a possible undertreatment of patients with biomechanically significant abnormalities.
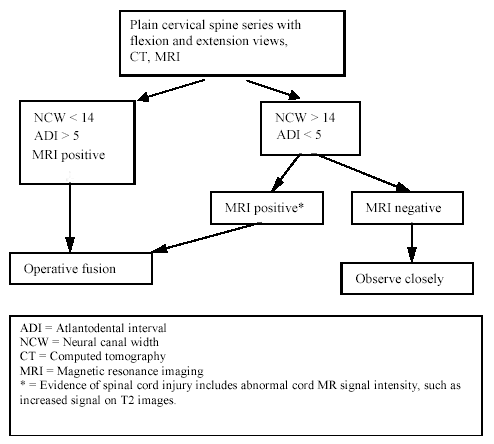 |
| Figure 2. Clinical management algorithm for symptomatic atlanto-axial instability in Down's syndrome |
Historically, the attempts at operative fusion in Down's syndrome patients have met with poor success. In two recent studies, Segal, et al.,23 (1991) and Doyle, et al.,7 (1996) together reported 21 major complications in 25 patients undergoing fusion procedures at the cranio-cervical junction. All of these patients underwent posterior arthrodesis with or without internal fixation. All of the patients also received external orthoses. These two studies obtained a 40% and 80% fusion rate, respectively.
Menezes and Ryken10 in 1992 described their operative experience in 18 patients, 10 of whom underwent occiput to C2 fusion and eight of whom underwent AA fusion. All of these patients achieved bony union with a minimum of complications. Our own experience at the Primary Children's Medical Center in Salt Lake City, Utah with five patients with Down's syndrome has been encouraging so far. We have used a combination C1-2 transarticular screw fixation coupled with a rigid, contoured titanium implant in order to obtain a rigid stable internal fixation construct.3 No halo orthoses were used in any of the patients we managed. So far we have had successful fusion in all of our cases. However, of the three complications in our case series (two wound infections and one screw backout), all have occurred in Down's syndrome patients. Although our initial results are encouraging, it is still too early to determine the longterm effects of such a procedure.
The following recommendations are based on an extensive review of the literature and careful study of the biomechanics of the craniovertebral junction and their significance. A careful history and physical examination should be performed by primary care providers on a routine basis for Down's syndrome patients with attention paid to myelopathic signs and symptoms. All patients who desire to participate in "high-risk" sports should undergo screening according to the Special Olympics guidelines. In addition, all patients who are undergoing otolaryngologic procedures should obtain preoperative screening studies as well. Most screening studies should be completed by approximately age five or six, or later if desired by the parents. The NCW and ADI should be measured in all patients. If the neural canal width is less then 14mm, then an MRI should be strongly considered.
Two treatment algorithms are provided for the clinical scenarios that neurosurgeons might encounter. The first, in patients with asymptomatic C1-2 instability, is seen in Figure 1. It emphasizes the detection of bony anomalies and aggressive work-up of this important subgroup of patients. It also relies on MRI to detect spinal cord injury in order to sort out which patients with AA subluxation should undergo operative fusion. Positive MRI findings include signal changes within the spinal cord that indicate subacute or chronic cord compression or injury (i.e. increased signal on T2 sequences).
The next clinical scenario, seen in patients with symptomatic C1-2 instability, is less complicated. This algorithm is seen in Figure 2. Again, it relies on plain films for screening for subluxation. If subluxation is present and the MRI is positive, operative fusion is indicated. However, there is a group of patients who are symptomatic nonsubluxators and MRI scanning should be helpful in defining this population. If the MRI is positive, then operative fusion is indicated, and if it is negative, close observation is necessary.
Finally, the presence of OAI is of uncertain significance and incompletely understood at this time. White and Panjabi state that greater than 2mm of subluxation in a normal adult should be considered grounds for instability.28 According to Menezes (personal communication, 1999), greater than 7mm of subluxation at the occipital-atlantal joint in Down syndrome is evidence of instability. Our policy at the Primary Children's Medical Center is that fusion should be recommended strongly in any patient with greater than 8- 10mm of subluxation at the O-C1 level. This recommendation is discussed very carefully and extensively with the family and all of the benefits and risks of surgery are fully covered. Until further information is obtained, protection of the neural elements and prevention of possible catastrophic accidents in grossly unstable OA joints takes precedence over the potential risks associated with surgery.