3.21 Three two one
Vol. 1, No. 6, December 1998
3.21 Three two one |
| |
|
3.21 A newsletter that examines the medical aspects of Down syndrome Vol. 1, No. 6, December 1998 |
Reprinted with the permission of Karalee Wetzel |
|
Help - looking for a journal I am looking for the subscription address or phone number for the Journal of Intellectual Disabilities Research. This is really the premier journal for disabilities, and probably half of what I use here I get from that journal. (Unfortunately, medical journals are usually close to $200 to subscribe to, but there is often a substantial student discount.) |
|
This edition Ear infections/hearing loss, tongue reduction: speech Next edition More on speech, cell therapy (is it effective/safe) |
Hearing loss is an extremely frequent problem for those with DS. One study looked at adults with DS. Depending on what criteria was used to define a loss, between 51-74% had some hearing deficiency (Keiser, et al. 1981). Another study found that children with DS had a 82.5% chance of having some type of hearing impairment compared to .5%-2% in the normal population. If one ignores cosmetic issues such as height and facial characteristics, hearing loss is probably the most frequently seen complication of DS.
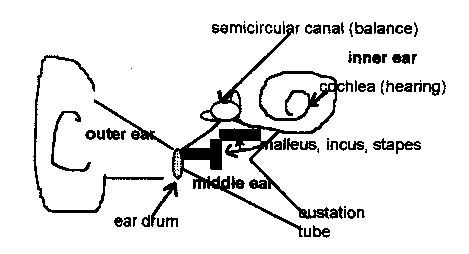
There are two general types of hearing loss. The first is having a nerve problem most likely from the 8th cranial nerve that carries both balance and acoustic senses. (There are other accessory nerves that can also affect hearing, but that is very complicated.)
The other major problem with hearing loss is called "conductive" and has to do with problems with the parts. Those equipment parts can be malformed at birth, can be damaged during trauma and aging, or what is seen commonly with children is they are damaged from ear infections. If that is the case, sometimes they are temporarily "stuck" due to the inflammation and secretions that come with ear infections or as doctors call it otitis media (OM).
If you look at the drawing above, please notice a few things. First, the extreme interconnection between hearing and balance. Not only are those nerves fibers carried on the same nerve, but the cochlea and the semicircular canals are attached to each other. That is why OM can make a person dizzy.
Second, notice the 3 bones (the incus, malleus and stapes) that are the "percussion" interconnection between the outer ear and the inner ear. Having seen those bones recently in gross anatomy, I can tell you those are not drawn to scale. In fact, once could barely see them. They are so delicate that any type of "mucking up" dramatically decreases their effectiveness.
Finally, the eustation tube can be problematic. It has a fairly direct link to the sinuses especially in small children. That is how frequent colds or runny noses or letting a child drink a bottle in a horizontal position can lead to ear infections. Ear tubes give the walls of the eustation tubes more rigidity and make the canal less likely to close up and keep infectious material in the middle ear.
One study compared the cause of hearing loss in DS versus other with mental retardation but no DS. They found that while the hearing-impaired non-DS group all have nerve problems, the DS group had mainly conductive type problems. Mainly those problems were in the middle ear and/or eustation tubes.
Additionally, the authors noticed the defects in the "pinna" or the outer ear that we see externally. Since they are funnel that carry the waves in, defects in those will certainly have an effect on hearing (Mazzoni, et al. 1994).
We know that kids with DS suffer from more OM, upper respiratory infections and are just more prone to bugs.
What is very scary is that many time kids can have OM and not have symptoms of discomfort or even signs that a physician could see in a routine look in the ear. One group looked at the mastoid air cells (via lateral radiographs) of kids with DS. Those air cells surround the middle ear. 42% of kids with DS had sclerosis of mast cells, which indicates untreated or inadequately treated OM. Nearly 1/3 of those had no history of known OM, so the authors believed that many of these kids had ear infections for awhile and no one knew. Destruction of mastoid air cells alone will not necessarily lead to hearing loss, but there is a strong link between OM and hearing loss. (Roizen, et. al. 1994)
The first line of action is of course prevention. For example, many pediatricians (and I believe the APA) recommend keeping children away from second hand cigarette smoke which is believed to cause about ½ of all ear infections. Also keeping those runny noses in check. If they get too bad or frequent, decongestants can be discussed with your pediatrician.
Frequent auditory screenings and tests for OM for children with DS are recommended. Hearing tests can be the quickie ones given at the schools or more sensitive brainstem evoked response. With very young children, the latter is the way to go.
To check for ear infections, beyond looking in the ear at each doctor visits, typanograms can often show there is congestion in the middle ear. After reading the research I did for this article that pointed out how many kids have undiagnosed OM, I would think a trip to the ENT every few years would be wise.
Antibiotics often work but often do not. Part of the problem is the middle ear is fairly enclosed an it is hard for the meds to physically get in there with enough power to kill the bugs. Echinacea is being used more often as the first line of treatment, and in Germany is the first med given to combat OM. The problem with meds is the bugs get smarter and a person hates to show all their arsenal tricks too early in the childhood years because something big may hit the kid later. There is also no good stats on antibiotic effectiveness in OM in DS.
The next defense is inserting ear tubes. That is a big decision for parents and is controversial as to when in the ear infection war does one try it. The decision is made tougher by the differences seen in outcomes in children with DS. Children with DS compared to children without for positive outcomes after having ear tubes placed due to chronic OM. While those without DS had about a 91% success rate, those with DS had only a 60% success rate (Selikowitz, 1993).
Hearing aides are usually the last option many parents want to take. The one fortunate thing is that unlike nerve problems, conduction problems often can be overcome by hearing aides. There are so many realistic issues with aides: getting kids to wear them, the cost, and the psychological issue of having one more thing people will tease my kid about. (One child I knew threw her aides out the bus window and flushed her next set down the toilet.) The upside is that research shows that kids with DS who hear better will have increases in IQ's, speech and social skills. So keeping on top of this hearing issue is a very big deal for the quality of living for kids with DS.
Keiser, et al. (1981) Hearing loss of Down syndrome adults. Am. J. Ment. Defic. 85(5) 467-72
Mazzoni, D. et al. (1994) Abnormal pinna type and hearing loss correlation in Down's syndrome. J. Intellect Dis. Res. 38(pt 6), 549-60.
Roizen, N. et al. (1994) Sclerosis of the mastoid air cells as an indicator of undiagnosed otitis media in children with Down's syndrome. Clin. Pediatre. Phil. 33(7), 439-43.
Selikowitz, M. (1993) Short-term efficacy of tympanostomy tubes for secretory otitis media in children with Down syndrome. Dev. Med. Child. Neurol. 35(6) 511-5.
When Jen was a baby, she did two things at night that would freak us (and the babysitters) out. First, she slept with her eyes half open. Not only does that look icky, but an cause damage to the eyes. The second thing she did was she slept with her head between her feet, or she would trash around violently, with what looked like efforts to get her mouth in the right position to breath. Every morning she would cough up white slime.
My husband and I had talked about plastic surgery for cosmetic reasons already. Anyway, we were able to not only rationalize it in our own minds but have insurance pay for it because of what was mentioned above with Jen's breathing, problems and eye problems.
I found a surgeon I was comfortable with, a Dr. Bill MaGee in Norfolk, VA. MaGee used to be a dentist before plastic surgery. He also started up the group Operation Smile where docs go around the world providing free medical services to children who cannot afford it.
MaGee told me he was willing to release the tendons around Jen's eyes and that should let her lids close while sleeping. It would also give her a more "normal" appearance by reducing the slant in her eyes. I had originally decided against tongue reduction because the research does not support it helps with speech. MaGee asked me about Jen's breathing and sleep, and suggested tongue reduction to not only correct the breathing problem, but to prevent teeth problems which result from the small mouths often seen in DS. I really resisted, but he was convincing and we agreed.
The operation was traumatic for Jen but probably worse for me. She looked awful, with huge stitches goes down her tongue (the eye was a breeze). Eventually, the trauma went away. Jen still has a scar, and it took a while for the tongue to get full range of motion back. Today, she sleeps fairly peacefully now with just some snoring, and there is no morning slime. The tendons in the eye have tightened up and the slant is coming back, but she can keep her eyes closed during sleep. I still get comments like "she must only have a little Down's" from strangers, which is what I want them to think.
Many parents of DS children not only questioned my thinking on it, but attacked us for using it, saying we were caving. What is interesting is that parents without DS children only supported that decision. Our only goal was to give Jen a chance at the most normal life possible.
After the long personal experience, I did want to share some of the medical research on tongue reduction and why any parent would put their kid through that. If any of you are even considering tongue reduction, please let me know. I will send you 24-hour post op photos of Jen that are pretty gross so an informed decision can be made.
One study followed 4 children with DS (age 20 mo. to 5 yrs.) who had undergone tongue reduction. All had constant tongue protrusion. 3 had obstructive airway problems, and 2 had feeding difficulties preoperatively. The surgery did improve appearance and airway function in all children. However, neither feeding nor speech problems were helped by the surgery (Morgan, et al. 1996)
A German group followed children with DS who also had the partial glossectomy. The authors stated that when the size of the tongue and mouth are not balanced, the following affects are seen: more infection (because of mouth breathing), drooling, difficulty chewing and drinking, and speech problems. This group say the following results of the 102 children who underwent the surgery.
93% had predominately open-mouth breathing before, and only 15% did after. 83% had colds more than 2 times/year before and only 22% did after. Parents also noticed improvement in speech, eating and attitudes by strangers towards their child (Olbrisch, 1982).
Another study used a variety of techniques to open airways including tongue reduction, reducing the ulva, advancing the tongue or jaw. All patients improved in terms of snoring, noisy breathing and oxygen requirements. (LeFaivre, et al. 1997).
The next study looked at the dental issues. It seems that Dr. MaGee was right in tongue reduction preventing teeth problems. Resting pressure that the tongue puts on the teeth was higher preoperatively in kids with DS who underwent tongue reduction, but the levels were lower and near normal 12 months after surgery (Frohlich, et al. 1993).
Tongue reduction is a major surgery, although all the studies I read described only minor complications. I would not recommend it if cosmetics is the only purpose. However, when airways are compromised, it beats tracheostomy (putting a tube in the trachea to breath through) which can be an option if the obstruction is too bad.
Frohlich, K. et al. (1993) Influence of surgical tongue reduction on pressure from the tongue on the teeth. Angle-Orthod. 63(3) 191-8.
LeFaivre, J. et al. (1997) Down syndrome: identification and surgical management of obstructive sleep apnea. Plas-Reconstr-Surg. 99(3) 629-37.
Morgan, W. et al. (1996) Surgical management of macroglossia in children. Arch-Otolaryngol-Head-Neck-Surg. 122(3) 326-9.
Olbrisch, R. (1982) Plastic surgery management of children with Down syndrome: implications and results. Brit-J-Plas-Surg. 35, 195-200.
|
Speech Suggestions In Jon Miller's writing that appeared in the book Down Syndrome: A Resource Handbook he gave the following suggestion for parents and siblings to facilitate speech in the family member with DS.
Down Syndrome: A Resource Handbook (1988). |